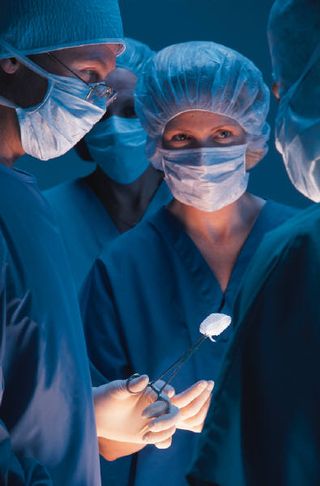
 [Pacemakers] prolong lives, but “all those people will face decisions down the road,” Dr. Mueller said. “’Do I keep it going? Do I turn it off?’” Physicians have similar questions, including what kinds of patients confront these choices and who usually winds up making these decisions.
[Pacemakers] prolong lives, but “all those people will face decisions down the road,” Dr. Mueller said. “’Do I keep it going? Do I turn it off?’” Physicians have similar questions, including what kinds of patients confront these choices and who usually winds up making these decisions.
Do you or a loved one live with a pacemaker or implanted defibrillator? These devices keep the clock ticking, so to speak. But when you are making end-of-life plans, when is the right time to turn the pacemaker off? This scenario is all too common and is presenting challenges in geriatric medicine and palliative care.
Recently, The New Old Age Blog took a look at this perplexing issue in an article titled “A Decision Deferred: Turning Off the Pacemaker.”
Compounding the problem is the fact that standard medical directives are designed with feeding tubes and breathing support in mind. Rarely do such legal instruments address the question of a pacemaker, implanted defibrillator or other surgically implanted electronic heart monitor. These devices may extend life, and maybe not for the better, but without the directive who is empowered to direct when or even whether they should be turned off?
Simply put: no one.
So how many patients with these devices have built their wishes (whether on or off) into their plans and medical directives? In one survey of 150 elderly and dying Mayo clinic patients, more than half had a medical directive (and only that — a bad statistic in itself). However, only one medical directive addressed the issue of the patient’s defibrillator.
Reference: The New York Times – The New Old Age Blog (January 29, 2014) “A Decision Deferred: Turning Off the Pacemaker”
 Houston Estate Planning and Elder Law Attorney Blog
Houston Estate Planning and Elder Law Attorney Blog